- COVID-19 Update: Our office is OPEN and scheduling patients. We are dedicated to keeping our patients safe & healthy.
Platelet Rich Plasma (PRP)
Platelet-Rich Plasma (PRP) Injection Therapy in Philadelphia
Regenerative Healing Powered by Your Body
At Greenberg Regenerative Medicine, we specialize in innovative regenerative medicine treatments that harness your body’s natural ability to heal. One of the most effective and versatile therapies we offer is Platelet-Rich Plasma (PRP) therapy—a safe, minimally invasive solution for pain, injury, and inflammation that uses components from your own blood to accelerate recovery.
Whether you’re suffering from joint pain, sports injuries, chronic tendonitis, or skin and hair concerns, PRP therapy can stimulate repair at the cellular level and support long-term healing.
What Is PRP Therapy?
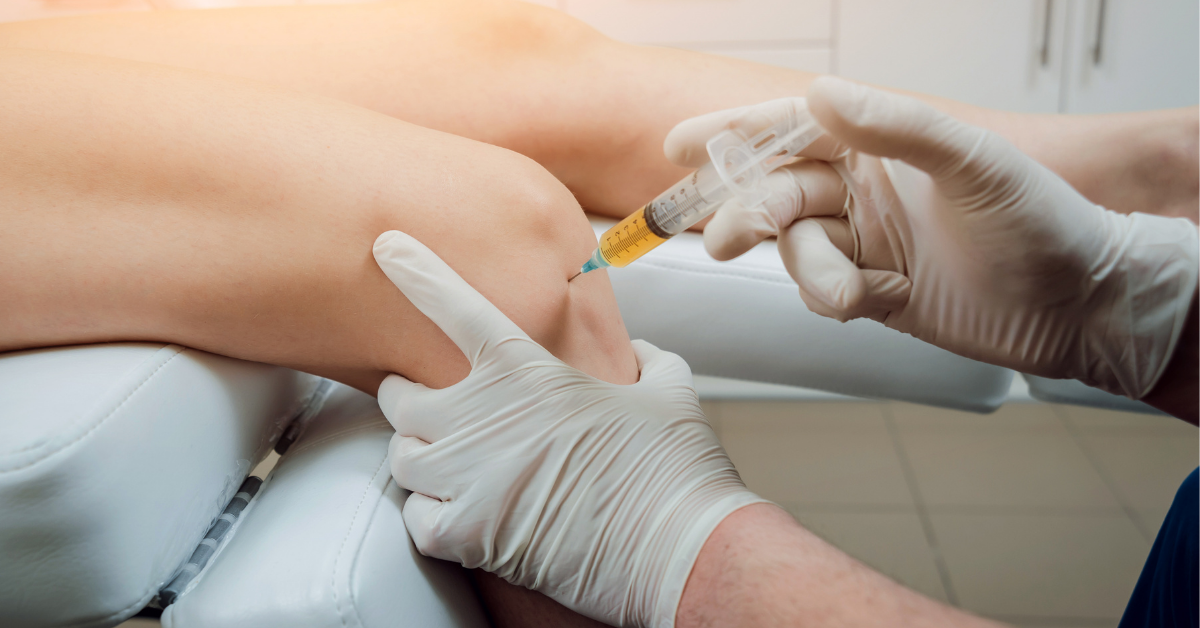
 PRP therapy involves drawing a small amount of your blood, processing it to isolate a high concentration of platelets and growth factors, and injecting it into the targeted area. Platelets play a crucial role in tissue regeneration and inflammation control, making PRP a powerful tool for treating musculoskeletal conditions, arthritis, and even cosmetic issues like hair thinning or aging skin.
PRP therapy involves drawing a small amount of your blood, processing it to isolate a high concentration of platelets and growth factors, and injecting it into the targeted area. Platelets play a crucial role in tissue regeneration and inflammation control, making PRP a powerful tool for treating musculoskeletal conditions, arthritis, and even cosmetic issues like hair thinning or aging skin.
Because PRP is derived from your own blood, the treatment is:
Autologous (from your body)
Low-risk
Free of synthetic additives or drugs
Conditions Commonly Treated with PRP
Greenberg Regnerative Medicine commonly treats a wide variety of ailments with PRP Therapy in their Bryn Mawr, PA offices. Patients from across the Philadelphia area and across the country have been treated with PRP injections by Dr. Scott Greenberg with many seeing positive results for a wide variety of ailments and conditions.
PRP is highly adaptable and can be used to treat a wide range of orthopedic, cosmetic, and systemic conditions, including:
Knee, shoulder, hip, and joint pain
Tendon injuries (tennis elbow, Achilles tendonitis)
Plantar fasciitis
Arthritis and degenerative joint disease
Sports Injuries and Strains
Upper and Lower Cervical Spine Disorders
Post-Concussion Syndrome
Headaches
Lower Back Pain
Spinal Stenosis
Herniated Discs
- Sacroiliac Joint Pan
PRP Therapy can help patients recover quicker from common injuries and ailments. Click below to see if PRP can help you!
What to Expect From PRP Therapy Treatment
PRP therapy is a minimally invasive, outpatient procedure, performed in a single visit with little to no downtime. PRP Therapy at Greenberg Regenerative medicine is typically performed in-office and takes about 60–90 minutes from start to finish. After your blood is drawn and processed, the Platelet Rich Plasma (PRP) is carefully injected into the affected area.
Most patients experience only mild discomfort and minimal downtime.
Click below to learn what to expect on the day of your procedure.
Ready to See what PRP Therapy Can Do For You?
Click below to book your appointment and explore PRP and other Regenerative Therapies with Dr. Greenberg. Our office is conveniently located just outside of Philadelphia in Bryn Mawr, PA.
Schedule an Appointment Today!
- (833) 440-4325
- info@greenbergregen.com
- 101 S Bryn Mawr Avenue Suite 300a Bryn Mawr, PA 19010