Acupuncture for Mental Health: Does it Work?
Learn about acupuncture, its benefits for mental health, and how Dr. Sadek provides this treatment.

Learn about acupuncture, its benefits for mental health, and how Dr. Sadek provides this treatment.

What is Alzheimer’s Disease? The Center for Disease Control (CDC) defines Alzheimer’s Disease as the most common type of dementia – in other words, the
Learn more about regenerative medicine treatment options for different types of arthritis.

Learn about recent developments and alternative methods to treating chronic pain without opioids.
With decades of research, treatments, trials, & success stories- stem cell therapy in 2022 is already proving to show even more great signs of alleviating pain.

You’ve seen them online, in your local drugstore, and maybe you’re already taking some! Supplements come in all shapes and sizes, for a wide range of health benefits, and it can be hard to decipher which you may need to add to your health regimen.
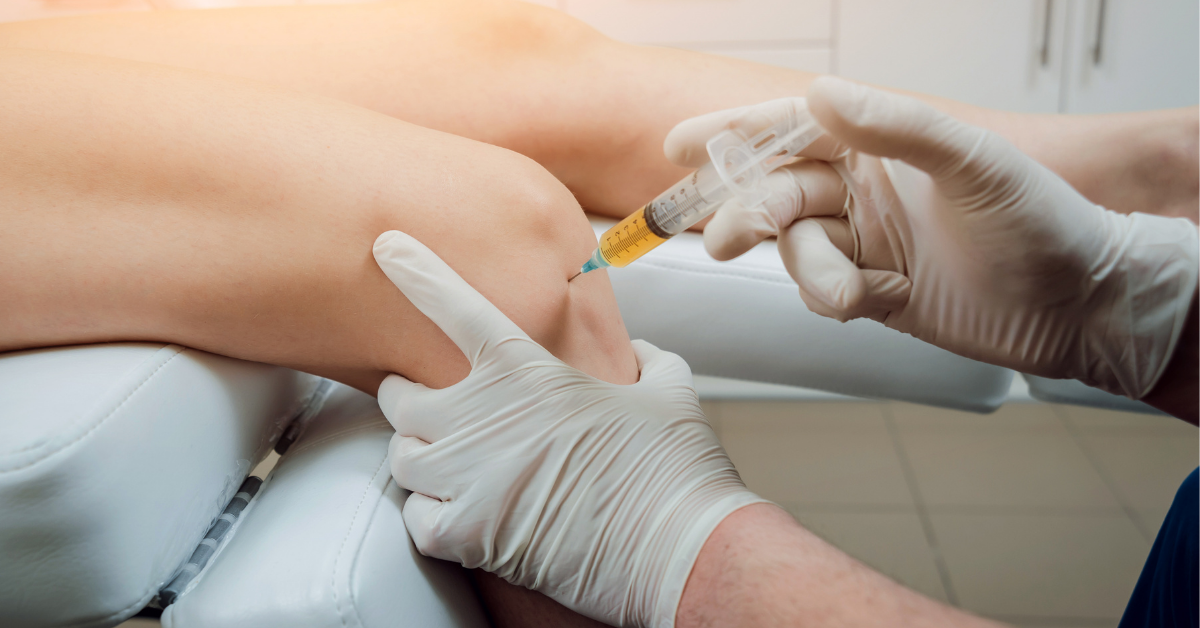
As patients try to treat the pain with cortisone shots, physical therapy, and as a last resort a myriad of surgeries, Platelet-Rich Plasma for the knee is often overlooked.

When it comes to lifting weights specifically, it is important to make sure you are protecting your body correctly to prevent unwanted injuries.

Through regenerative medicinal practices, Dr. Greenberg often recommends Platelet Rich Plasma injections to amplify healing & provide relief for his patients.

In September Scott Greenberg, MD had the opportunity to present to the doctors and fellows at The Marcus Institute of Integrative Health at Jefferson Health located in Philadelphia, Pennsylvania.